Health, Fitness, Diet, & Nutrition Blog Dedicated
to your well-being (Est. Since 2010)
Can YOU prevent health problems, cancer, disease, and illness through healthy foods, fitness, and a more relaxed lifestyle?
Public health organizations are now seriously concerned about health risks associated with dietary exposure to cancer-causing metals!
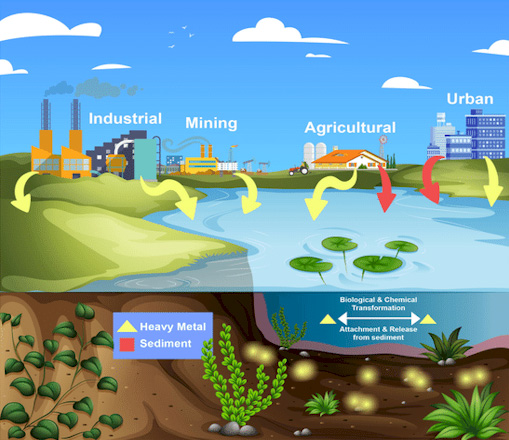 Food crops can absorb heavy metals from contaminated soil, air, and water. Foodbourne metal contamination is now a serious concern of public health officials, although their concerns are being aired, somewhat quietly.
Food crops can absorb heavy metals from contaminated soil, air, and water. Foodbourne metal contamination is now a serious concern of public health officials, although their concerns are being aired, somewhat quietly.
Despite this, there has been exceptions. Recently US Congressional Report detailing high levels of metals found in infant food pulled off grocery shelves, is one of them, and another with the discovery of high levels of lead being found in children's fruit puree pouches.
These are a few cases that were publically discussed and concerned many people in US and even Canada, a major trading partner of US that purchases food made here.
Health risks of dietary exposure to lead, arsenic, and cadmium are very concerning, especially to public officials in North America. Data gathered by researchers on the dietary intake of each metal from various sources such as food and water samples have caused alarm and resulted on more existing studies and reports coming out regarding this. The researchers analyzed the data and were surprsed of the severity of the problem.
Arsenic is readily found in rice, wheat, and leafy green vegetables, among other foods. Arsenic research studies for the last 3 decades has demonstrated moderate to high scores for skin, bladder, lung, kidney, and liver cancers.
... More >
Excess body weight isn't a cosmetic concern. It's a medical problem that increases the risk of many life-thretening diseases and health problems.
 Excessive body weight and obesity is alarmingly increasing, and now a major US public health issue. US alone has witnessed a triple escalation since the year 2000. Bad diet, sedentary lifestyle, fast-food culture and the increase in consumption of high-calorie processed food.
Excessive body weight and obesity is alarmingly increasing, and now a major US public health issue. US alone has witnessed a triple escalation since the year 2000. Bad diet, sedentary lifestyle, fast-food culture and the increase in consumption of high-calorie processed food.
The alarming increase in childhood obesity discussed by public officials demonstrates a tremendous burden of chronic disease awaiting the public healthcare system here in US and even in Canada.
Massively overweight and obesity prevention through weight loss programs are critical factors in controlling excessive-weight related diseases, including diabetes, cardiovascular disease, stroke, hypertension, cancer, and psychological problems.
Even our healthcare professions themselves are not immune, and mnny of whom are overweight, some severely. Long working hours and stressful life is causing fatigue.
Who time to cook, eat nutritious food, or exercise? Obesity is strongly connected to fast foods, processed foods, and lack of moderate excersize due to not being able to find time to relax and rejuvanate.
Americans are still not demanding that the public health authorities recommend strategies for the management and prevention of this major health concern.
... More >
